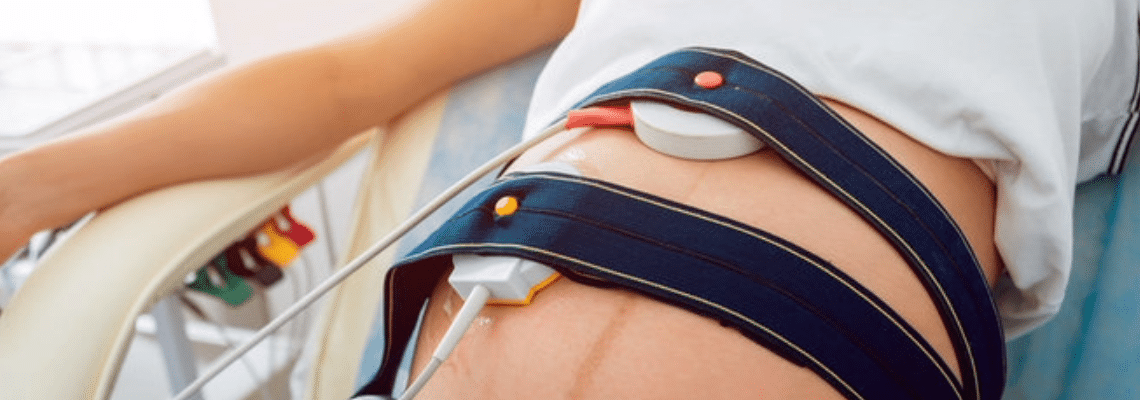
Cardiotocography (CTG) refers to the electronic recording of the fetal heart rate and contractions. The fetal heart rate recorded over the mother’s abdomen is the most commonly used method for monitoring the fetus during labor. A research team from the University of Helsinki and Helsinki University Hospital (HUS) has found that external monitoring of the fetal heart rate without simultaneous recording of the maternal pulse is associated with an increased risk of both neonatal encephalopathy and acidosis in the blood of the fetal umbilical artery, i.e., critically low pH levels and high concentrations of base excess. Acidosis increases the need for neonatal resuscitation and prolongs the duration of intensive care. The study, published in the renowned American Journal of Obstetrics and Gynecology, analyzed nearly 214,000 spontaneous full-term births at HUS maternity clinics between 2005 and 2023. The study included the largest CTG dataset ever published.
External Monitoring
The study showed that among newborns monitored exclusively via external fetal heart rate monitoring during labor, the risk of neonatal encephalopathy was 1.6 times higher and the risk of severe umbilical cord blood acidosis was 2.3 times higher than among newborns monitored with an internal electrode attached to the skin of the fetal head (internal monitoring) or through simultaneous external fetal heart rate monitoring and recording of the maternal pulse.
“Especially during the second stage of labor, when mothers tend to have an elevated heart rate while pushing, fetal heart rate decelerations occur more frequently. Consequently, the fetal heart rate can quite easily be confused with the maternal pulse; in this case, abnormal fetal heart rate tracings indicating fetal hypoxia may be overlooked by healthcare professionals,” explained researcher Mikko Tarvonen, outlining the challenges of external CTG monitoring. In the majority of births in the study (38%), external monitoring was used exclusively. Internal monitoring was the second most common method (33%), followed by external monitoring combined with maternal pulse recording (29%).
Encephalopathy in Infants
In newborns, a specific form of encephalopathy is often referred to as hypoxic-ischemic encephalopathy (HIE). It is usually caused by a lack of oxygen during or shortly after birth, for example due to complications such as umbilical cord entanglement, placental problems, or difficult deliveries. The lack of oxygen damages the sensitive brain tissue, which can impair normal development.
Symptoms often appear shortly after birth and can range from feeding difficulties, muscle tone disorders, and excessive sleepiness to seizures or impaired consciousness. The consequences depend heavily on the extent of the damage: In mild cases, children can recover well; in more severe cases, there is a risk of permanent developmental disorders such as motor impairments or learning difficulties. Early treatment—for example, through controlled cooling of the body—can help limit brain damage and improve the prognosis.
Years of Safe Practice at HUS
The world’s largest organizations of obstetricians and midwives recommend in their guidelines on fetal monitoring that external fetal heart rate monitoring be used as the primary CTG recording method. However, the new study shows that this method, without simultaneous recording of the maternal pulse, represents a significant risk factor that predisposes the fetus to birth-related hypoxia and its long-term neurological consequences. “Based on our findings, this tragedy can be effectively prevented by combining maternal pulse recording with fetal heart rate monitoring. This method allows healthcare professionals to be certain whose heart rate they are monitoring,” said Tarvonen. In 2019, HUS introduced a new protocol emphasizing the need to record the maternal heart rate alongside the fetal heart rate during childbirth. “Practices in Finnish maternity clinics have long varied, but training and research findings have led to a shift in thinking and, consequently, to increased use of maternal heart rate monitoring in recent years,” said Tarvonen.
The present study has shown that external fetal heart rate monitoring combined with maternal heart rate recording is just as safe as internal fetal monitoring in terms of the incidence of neonatal encephalopathy. However, internal monitoring proved to be the most accurate method for assessing fetal well-being. Its use was associated with the lowest incidence of hypoxia-related neonatal complications. The incidence of both neonatal encephalopathy and severe umbilical artery acidosis has decreased significantly in the HUS region during the study’s 18-year follow-up period. “This trend is exceptional even by international standards,” Tarvonen emphasized.
Facts: Monitoring the Well-Being of the Unborn Child Using Cardiotocography (CTG)
- Cardiotocography (CTG) refers to the electronic recording of the fetal heart rate and uterine contractions. The CTG recording is used for the early detection and prevention of fetal hypoxia during labor. Abnormal patterns—such as a persistently too high or too low heart rate or certain changes during labor—can be indications of a potential risk. In such cases, further measures can be taken to prevent or treat complications such as encephalopathy caused by oxygen deprivation in a timely manner.
- In Finland and other industrialized countries, CTG monitoring is the most common technique for fetal monitoring and is routinely performed during hospital births.
- CTG monitoring can be performed in three ways during labor: 1) by monitoring the fetal heart rate with an external ultrasound transducer attached to the mother’s abdomen, 2) using an external ultrasound transducer to monitor the fetal heart rate while simultaneously recording the maternal pulse, and 3) with an internal electrode attached to the skin of the fetal head.
- The latest CTG monitors allow for the recording of the maternal pulse via a uterine contraction sensor, eliminating the need for additional sensors.


