Guest Author: Dr. Linda Burke-Galloway, MD
One of the most important decisions you will make as a pregnant woman is where to have your baby. Most women will select a hospital although other options for birth include delivering at a birth center or for others, to deliver at home. Should you decide to give birth at a hospital, it is important for you to select the right one because they are not all made equal. Some look very pretty on the outside but have some patient safety concerns on the inside. Others might not look attractive externally, but you’ll receive the best care possible.
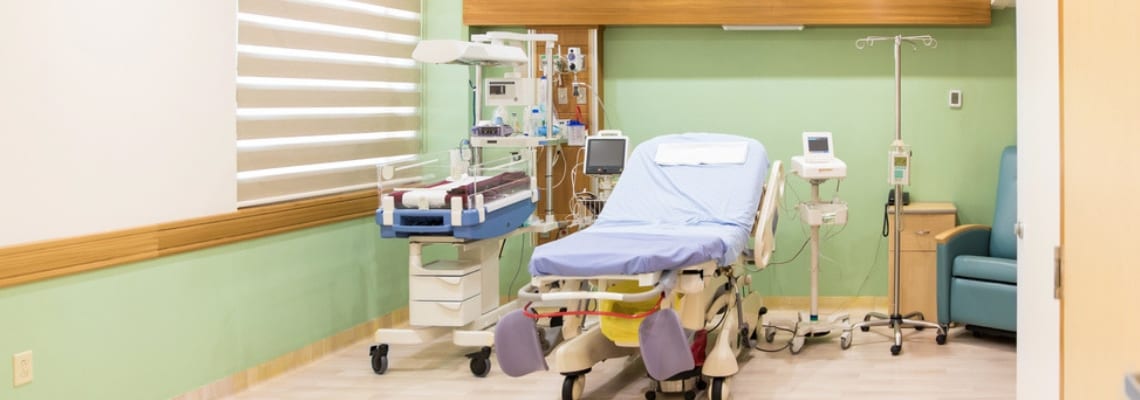
As a pregnant woman, one of the most important hospital features you should be concerned is its nursery. The type of neonatal nursery the hospital has, is extremely important, if your baby requires special care after it is born.
Three types of hospital nurseries provide neonatal care:
A level I nursery provides basic neonatal care and is the minimum requirement for any facility that offers inpatient maternity care. The hospital must have the personnel and equipment to perform neonatal resuscitation, evaluate healthy newborn infants, provide postnatal care, and stabilize ill newborn infants until they can be transferred to a facility that provides intensive care.
In addition to basic care, a level II nursery provides specialty neonatal care (sometimes called intermediate neonatal care). The nursery can provide care to infants who are moderately ill with problems that are expected to resolve rapidly or who are recovering from serious illness previously treated in a level III nursery.
A level III nursery, or sub-specialty neonatal intensive care unit (NICU), can care for newborn infants who are extremely premature, who are critically ill, or who require surgery.
Should an unforeseen emergency arise, the type of nursery your hospital has is extremely important. There have been unfortunate cases where extremely preterm babies were delivered at Level II hospitals and could not be transferred to Level III hospitals because of a shortage of beds.
If you develop a complication that could become worse (such as a blood pressure or a fever that keeps rising), your physician needs to make arrangements as soon as possible to transfer you to a hospital where both you and your baby will receive the best possible care.
Staff and Ranking
 In addition to looking at the hospital’s nursery, you need to ask the labor and delivery suite’s nursing director questions like these:
In addition to looking at the hospital’s nursery, you need to ask the labor and delivery suite’s nursing director questions like these:
- What is the nurse-to-patient ratio? Does one nurse have to take care of six or seven patients alone? While the nurse is attending to an emergency, who is going to be watching my fetal monitor or taking my vital signs?
- Does the hospital have a nursing shortage? Is it constantly short-staffed? (Ask former patients who delivered at the hospital.) What is the turnover rate? Are nurses constantly quitting and, if so, why? Are there enough nurses in the nursery?
- Are the labor and delivery suites overcrowded? If you make an unannounced visit on the labor floor, do you see patients lined up on the hallway? Sometimes, delivery beds will be at a premium, but this should be an exception rather than the rule. Overcrowding usually indicates a chronic shortage of beds and a hospital administration that is either insensitive to the problem or ill-equipped to deal with it.
Birthing Centers
If you are attended to by a midwife, your delivery might occur at a birthing center. A birthing center is a medical facility, often associated with a hospital, that is designed to provide a comfortable, homelike setting during childbirth. It may be part of the hospital campus or a separate stand-alone building. A birthing center should have the facilities to accommodate an emergency cesarean section, should the need arise.
Teaching Hospitals versus Community Hospitals
Teaching hospitals that have resident physicians offer a special benefit. You are fortunate if you will deliver at a teaching hospital because someone will always be available to deliver your baby in the event that your physician or provider is unavailable. This is not always the case at non-teaching hospitals or at hospitals in remote communities.
In addition, teaching or university-affiliated hospitals practice greater accountability than do non-teaching community hospitals and give patient management greater scrutiny, which is advantageous for everyone, especially the patients. Teaching hospitals have department chairpersons who have usually published articles in medical journals, teach in a medical school, or conduct clinical research. More importantly, teaching hospitals usually have “grand rounds,” in which all of the admitting and resident physicians discuss cases of interest as well as problem cases.
Dr. Linda Burke-Galloway is a board-certified ob-gyn physician with 30 years of clinical experience, author of a prenatal book and blogger who is passionate about teaching people how to understand their health conditions in order to obtain the best treatment possible. She is an alumnus of City College of New York, Columbia University School of Social Work and Boston University School of Medicine. In addition, she’s earned a certificate in Clinical Informatics at the Johns Hopkins School of Medicine. She is also a proud mother of two amazing sons and an international adoption advocate. Originally from Brooklyn, N.Y., she presently lives in Florida.


